To Make a Long Story Short ...
by Eric and April
 he story of Sarah's birth is unique in our experience as parents. Never before had we planned a hospital birth, and never before -- despite two C-sections and an induction -- had we spent so much time in the clutches of the medicalized birth machine that we had so sought to avoid as home birth parents.
he story of Sarah's birth is unique in our experience as parents. Never before had we planned a hospital birth, and never before -- despite two C-sections and an induction -- had we spent so much time in the clutches of the medicalized birth machine that we had so sought to avoid as home birth parents.
We want to tell this story in full, but it's a long one. At the same time we're eager to share the news of Sarah's birth, so first we'll make a long story short, then we'll take the time to tell it all.
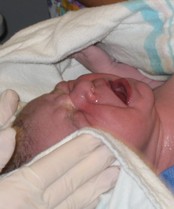
So the nutshell is that Sarah Paraskeva Scheidler was born on Friday, June 1, 2007 at 12:13 p.m. at Rush Hospital in Chicago, after a labor of approximatley 61 hours. April's labor was jinxed when her modest anxiety over giving birth in a hospital was enflamed into radical self-doubt by certian grim experiences upon first arriving at the hospital and being sent away again. In the end, it took pitocin and an epidural anesthetic to bring Sarah into the world.
There were many adventures along the way. The woman in the next curtain area who was told her baby had not heart beat and began to wail. The nurse who rolled her eyes at April's intent to avoid a C-section. The young resident physician who suggested the baby's head migh too big. The humorless pediatrician who coerced us into consenting to unnecessary tests we didn't want.
There was also the nurse named Noelle -- "Christmas" -- who settled us in when we were finally admitted, and who had had a home birth some 28 years before and was on the same page with us about natural birth. There were the many other excellent, comforting, thoughtful nurses we encountered in shift after shift in the labor and delivery ward. And the three attending physicians who each gave us their time generously and were very reassuring and clearly took our case very much to heart.
And above all, there was the birth of our new daughter Sarah Paraskeva Scheidler, who in the end was worth all the difficulties we had to face over these three longest days of our lives.
And now for those who want to hear the whole story in all its details . . .
Home Birth Not an Option
When we learned we were pregnant way back in September, our first thought was to try for another home birth. Nate, Sam, Clare and Ada were all born at home, and the experience was infinitely more pleasant than Liza and Mary's C-sections or Lucy's induction. Little did we know what was in store for us.
In December, April met with a doctor at Homefirst who was very encouraging about her prospects for a home birth despite having had two C-sections, including her last delivery. But at her January appointment -- with a different doctor -- concerns were raised, and she was refered to a practice at Rush that specializes in high risk pregnancy.
It wasn't until March -- during which time April was receiving no prenatal care -- that we were able to meet with Dr. Michael Hussey of Women's Health Consultants to discuss the possibility of having a VBAC.
Dr. Hussey explained the risks -- uterine rupture in particular -- but was very encouraging about April's prospects considering her three successful VBAC's in the past, her overall health and her high motivation. However, he suggested that natural birth in the hospital would be a safer course than home birth, so that in the unlikely event of a rupture, surgical care would be immediately available.
Planned Hospital Birth
And so for the next three months, Eric took time off of work every two weeks, and then every week, and finally twice a week to take April to the Professional Building at the Rush Hospital complex on the near west side of Chicago -- a drive of forty-five minutes in light traffic, which in heavy traffic could take as much as two hours.
This was a new experience for us -- to plan a hospital birth right from the start, and to receive care from a high risk obstetrics practice rather than a midwife or NFP-only family practice doctor. Strange to sit in a sleek waiting room filled with glossy parenting magazines, rather than our own doctor's humble office with it's tattered Dr. Suess books and back copies of CCL's Family Foundations. Unsettling to sit in examination rooms filled with contraception propaganda, in contrast to the yellowed clipping's about NFP and breast feeding we were used to.
But the care we received there was excellent, and Dr. Hussey and the other of the doctors they got to meet, Dr. Howard Strassner, continued to be encouraging and generous with their time. In fact, Dr. Hussey agreed to change the due date from May 13 to May 20 based on our certainty as to the date of conception -- a great relief, since April typically goes quite late.
In the final weeks of her pregnancy, April was required to visit the practice twice a week, once for her regular appointment, and once for an ultrasound to be certain the baby was still doing okay after the due date. It was late in the evening after their second "bio-physical profile" ultrasound (8 out of 8, by the way), that April woke up with strong contractions.
The Long Labor Begins
The contractions started about 11:00 p.m. After the third one, April asked Eric, who was still up reading, what time it was. It was by then 11:40, and for the next two hours or more we timed contractions and talked about what to do.
Our first concern was how long the drive to Chicago might take during rush hour. We knew well that this was only the very beginning of labor, and April's labors tended to be long anyway (the shortest was nine hours, the longest more than thitry). And yet their doctor had insisted that they come to the hospital as soon as there was as much as an hour of regular contractions so that the baby's heart rate could be monitored, the best indicator of uterine rupture.
We decided to get a few more hours sleep. Eric set the alarm for 5:00, so we'd have enough time to beat morning traffic if the needed to.
At 5:00 we awoke and took stock. April had continued to have contractions, but they were not very close together, maybe fifteen minutes. We decided to wait out rush hour and went back to sleep for a few more hours.
A Healthy Adjustment
Once we were up -- quite exhausted from a night of broken sleep -- April asked Eric not to go into work. He worked from home on his laptop as April's contractions continued as they had. Later in the morning we called Eric's mother Ann to come and get the kids, just in case.
Then we made a trip to the Healthy Futures Chiropractic. Dr. Dan Purdue had been treating April through the final months of her pregnancy, starting with a successful employment of the Webster Technique, which turned the baby head down; she had been in a breech position when an ultrasound was done in April. Dr. Dan went out of his way to fit us in before Ann came to get the kids.
After the chiropractic adjustment, contraction became much more frequent -- every seven minutes. So once the kids were off with their grandmother, we gathered our bags and drove downtown.
Triage Room from Hell
Note: Hereafter the narrative gives way to notes that will be filled out when Sarah's still-exhausted parents can find the time.
Drive to Rush, dinner, Triage room, sent back home to aurora
Going to adoration, talking to Dr. Pombar, and returning to Rush
Settled into Labor and Delivery room, nurse Noelle, meet with Dr. Pombar
Longest day of our lives; walking, trying to sleep. Meet with Dr. Strassner. Nap. Dr. Hussey. Nurses scarce. Moved to new room.
Water breaks, back to new labor and delivery room, try to get some sleep.
Morning: contractions have continued more regularly. But April so exhausted. Meet with Dr. Pombar again.
Decision taken: Get an epidural, then try some pitocin to augment the inadequate contractions.
Anesthesiologist pushes experimental treatment. Declined. Pitocin kicks in. read tobit
april notices anesthetic "blind spot". Anesth. called, plus resident. He checks april and finds she's fully dilated. On her next contraction, she pushes. In the middle of the next one, in walks anesthetist, then Dr. Pombar. Next contraction, baby born.
Pediatricians wash baby. placenta delivered. april breast feeds baby.
after an hour, baby taken away, bath refused. april sends eric to find out where she is and when she'll be back. fight with doctor over formula, hearing test, hepatitis b vaccine.
Eric returns to april, then goes back to baby for an hour while "heating" and waiting for test results continues.
eric rejoins april for transfer to new room; baby arrives shortly thereafter. grandma comes with the kids, and eric gets goofy. vandalizes silly note on bassinet. then try to get a good night's sleep.
saturday morning: pacing around waiting to leave. dr. comes again to argue about hearing test; claims we'll have to wait to be released if we don't go ahead with it. eric caves. then dr. chides him for note vandalism!
baby taken for hearing test -- immediately after eric got her back to sleep! baby returned, test results all finished, released! drive back to home and normal life.
Share Your Story Too
Homebirthers like us always meet lots of other folks with their own stories of both horror and joy. It's great to talk to people who can understand an experience like this. Please share your story at Eric's blog, Square Zero.